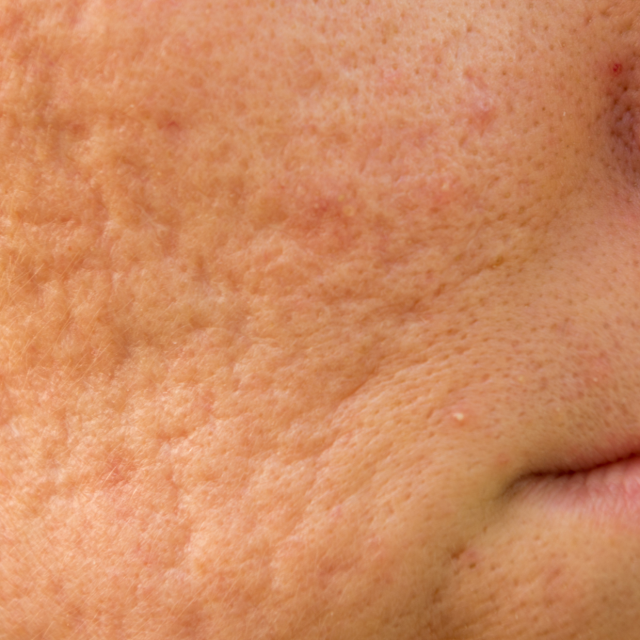
For many people, acne isn’t just a fleeting teenage issue—it leaves behind scars that serve as a constant reminder of past skin struggles. Acne scars can deeply affect confidence, self-esteem, and overall quality of life. At SRGN Clinic, we specialise in advanced, non-surgical acne scar treatments to effectively reduce the appearance of acne scars
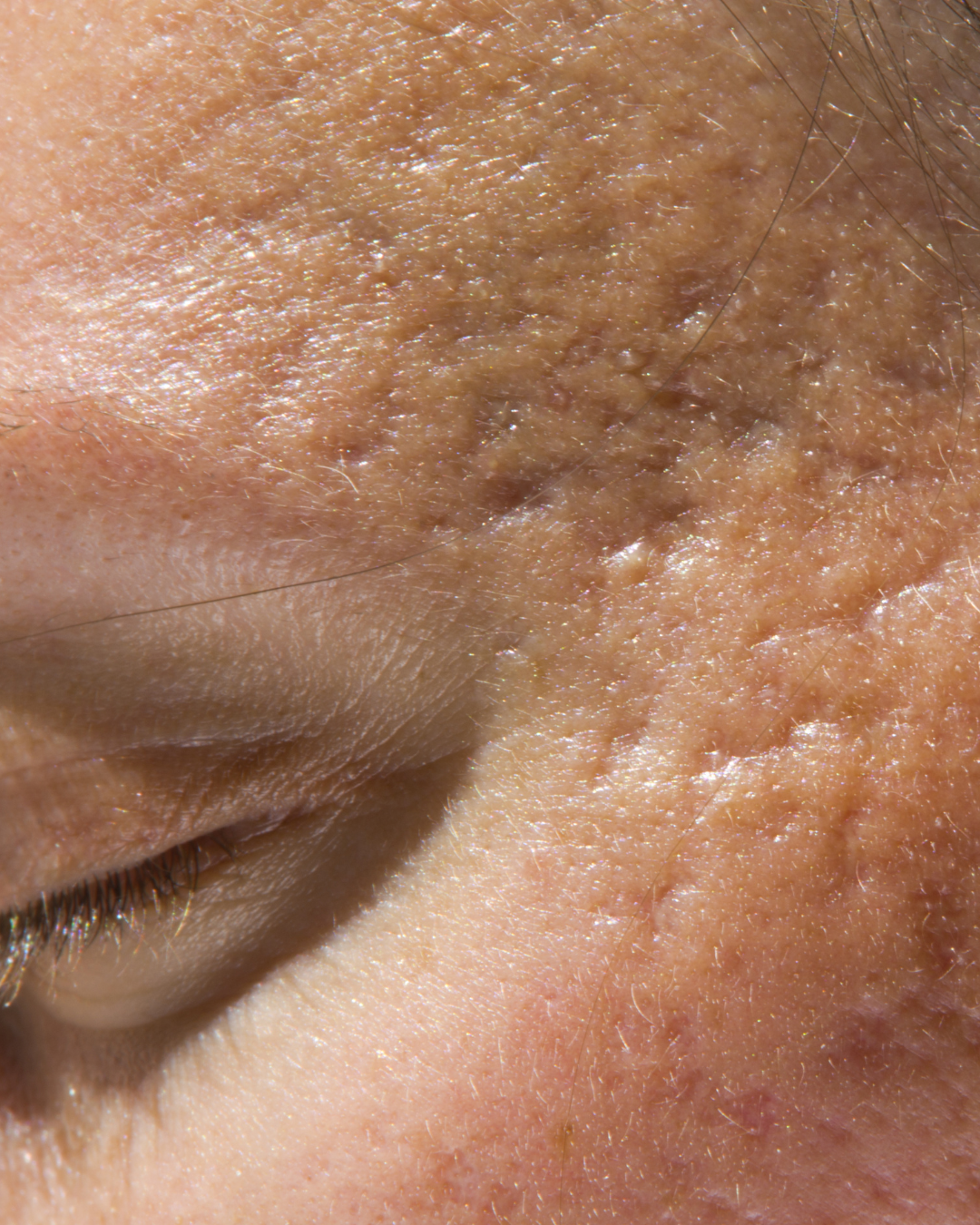
Acne scars are the visible marks left behind after acne lesions have healed. When acne damages the skin, the body attempts to repair it by producing collagen, a key protein that helps maintain skin structure. However, if collagen is overproduced or underproduced during the healing process, the result is scarring, so many start to seek an acne scar treatment.
When spots, such as acne, are picked or inflamed, they often lead to post-inflammatory hyperpigmentation (PIH). This form of hyperpigmentation appears as dark or discoloured marks left on the skin after the healing process. Although PIH is not a true scar, it can be stubborn and persistent, especially in darker skin tones, where melanin production is more reactive to inflammation. This makes it a frequent concern for those seeking an even complexion after acne or other skin injuries, and the solution lies in hyperpigmentation treatment.
The scarring process is influenced by various factors. Acne itself can trigger a complex inflammatory response that, if not properly managed, leads to scar formation. The severity and type of scars depend on a combination of factors, including:
Each of these factors contributes to the formation of scars that can be long-lasting, often creating a daily reminder of previous skin struggles. However, acne scars are highly treatable, and the right professional approach can make a lasting difference.
CO2 laser resurfacing is a highly effective treatment for reducing acne scars, and improving skin texture and overall complexion. The laser works by stimulating collagen production and resurfacing the skin, helping to smooth out uneven areas caused by scarring. This advanced technology targets deep into the skin to promote healing and regeneration, resulting in a clearer, more refined appearance. Ideal for mild to severe acne scars, CO2 laser treatment offers long-lasting results with minimal downtime.
SylfirmX also utilises microneedling and radiofrequency energy, but it employs a more targeted approach that’s effective for a variety of scar types, including both atrophic and hypertrophic scars. The radiofrequency energy reaches the deeper layers of the skin, triggering collagen and elastin production while breaking down scar tissue. This treatment not only improves the skin’s texture but also enhances resilience, creating smoother skin that appears refreshed and renewed.
Chemical peels are an ideal solution for those with superficial acne scars or pigmentation issues. By applying a customised chemical solution, we can remove the outer layers of skin, revealing smoother skin beneath. Chemical peels can also promote cell turnover, which gradually reduces scar depth and improves skin tone. The treatment is highly effective for post-inflammatory hyperpigmentation and can be tailored to address various types of scars.
Dermal fillers, specifically hyaluronic acid-based fillers, can be strategically used to fill in depressed scars like boxcar and rolling scars. By adding volume under the skin, dermal fillers smooth out the skin’s surface and diminish the appearance of indentations. This treatment provides immediate results, though occasional touch-ups may be required to maintain a lasting effect.
Dracula Facial therapy is a regenerative treatment that uses the body’s own growth factors to promote skin healing and collagen production. For acne scars, Dracula Facial injections can accelerate cell regeneration and improve skin structure, leading to a smoother texture. This natural approach is effective for a variety of scar types and provides long-term improvement in skin quality without introducing synthetic substances.
The best treatment depends on the scar type. SylfirmX microneedling with radio-frequency is effective for various scars, while chemical peels work well for surface marks, and dermal fillers can lift deeper, depressed scars.
Yes, many treatments can significantly reduce or even eliminate acne scars over time, though results vary depending on the scar's depth and treatment used.
Natural methods, like using vitamin C and regular sunscreen, can help fade superficial scars, but deeper scars often benefit from professional treatments for the best results.
Regular use of vitamin C, retinol, and sunscreen can gradually fade post-acne marks. For quicker results, consider treatments like chemical peels or RF microneedling.
Yes, vitamin C can help lighten dark spots and improve skin tone, making it useful for reducing the appearance of post-acne marks.
One week may be too short for complete removal, but treatments like dermal fillers can provide instant improvement in the look of depressed scars, while others take longer to show effects.
Dermal fillers offer immediate results for certain types of scars. Chemical peels and RF microneedling also deliver faster results, but may need a series of sessions.
Three days is a short window, but using a vitamin C serum and hydrating the skin can make marks appear less prominent. Lasting improvement, however, takes more time.
This varies by scar type and treatment, but typically, noticeable improvement may take several weeks to months. Complete scar removal, if possible, often requires multiple sessions.
Perceptions vary, but many people live confidently with or without scars. However, effective treatments are available if you wish to reduce their appearance.
Salicylic acid can help smooth skin texture and reduce pigmentation but is more effective for acne prevention than for treating deeper scars.
Acne marks may persist due to sun exposure, lack of consistent skincare, or because deeper scars require more intensive treatments like Dracula Facial, RF microneedling or chemical peels to improve.