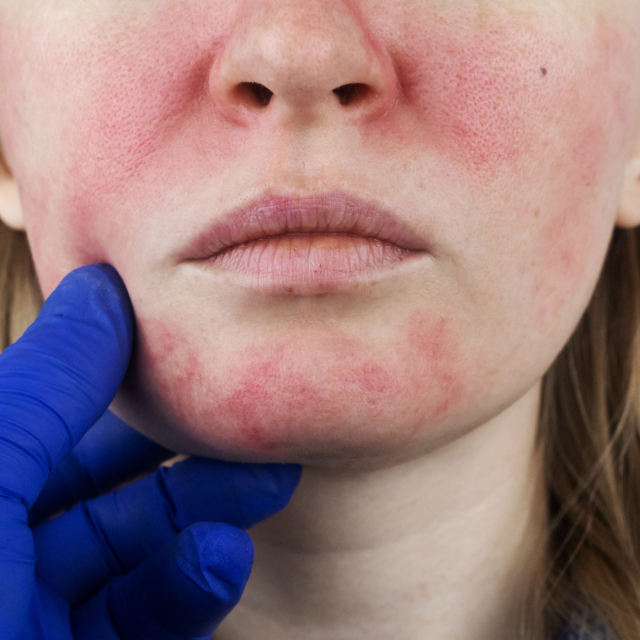
Living with chronic redness can be challenging, both aesthetically and emotionally, as the condition may feel unpredictable and difficult to cover with makeup or skincare products. At SRGN Clinic, we’re dedicated to helping clients manage it effectively through advanced, tailored treatments that target both the symptoms and underlying causes.
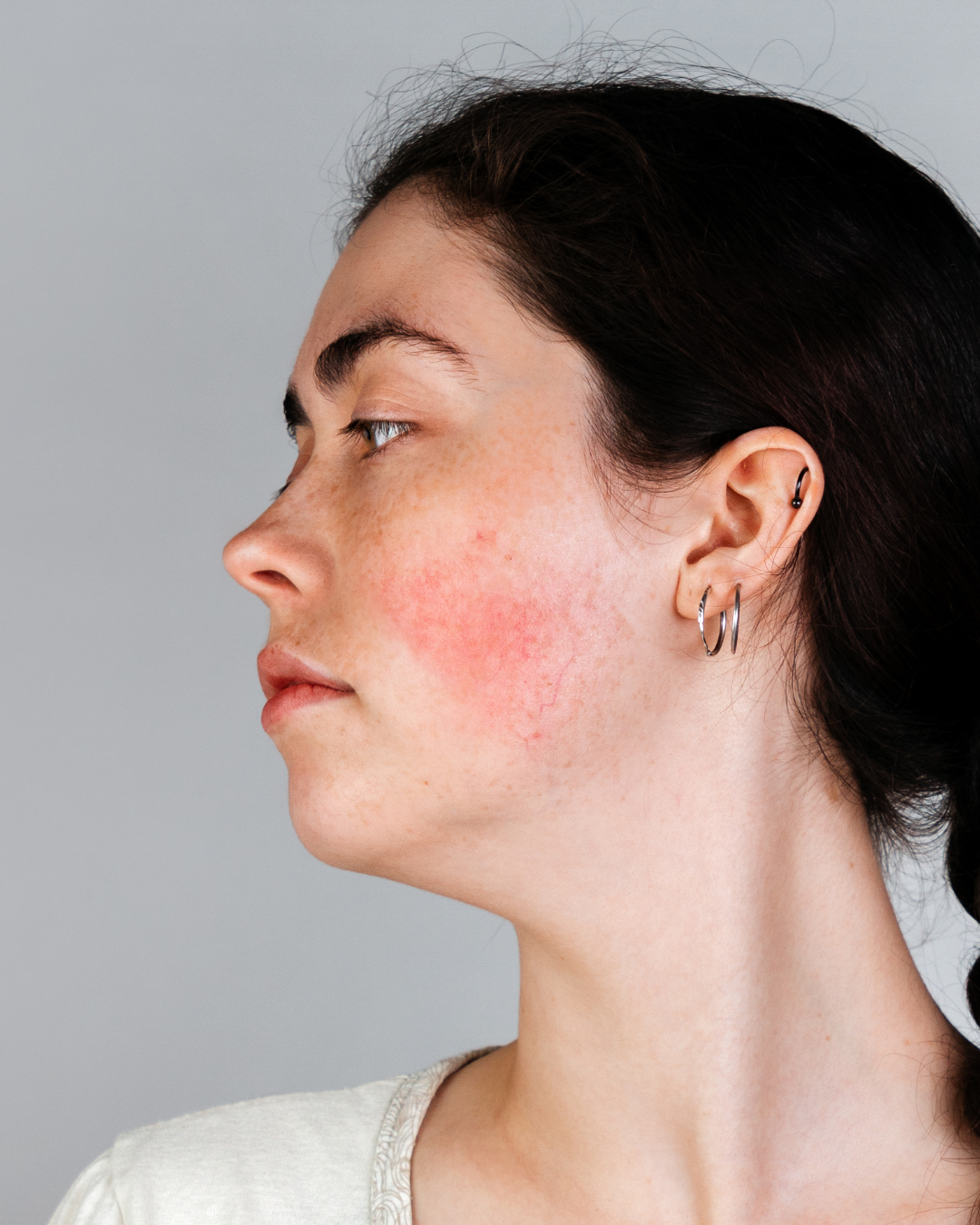
Redness in the skin occurs when blood vessels dilate or expand in response to internal or external triggers, leading to a visible flush or, in some cases, intense redness. This dilation allows more blood to flow to the skin’s surface, creating a red or pink appearance. For some, it is temporary, occurring after exercise or exposure to heat. However, chronic redness may be the result of more complex conditions, such as rosacea, which causes persistent redness, small visible blood vessels, and sometimes acne-like bumps on the face. Sensitive skin, prone to irritation from certain skincare ingredients or environmental factors, can also lead to frequent redness and discomfort.
It may also develop in response to inflammatory skin conditions like eczema or dermatitis. These conditions trigger the skin’s immune response, causing inflammation and redness that can worsen if untreated. Additionally, lifestyle factors like sun exposure, stress, diet, and even spicy foods can aggravate redness, particularly for those who are genetically predisposed to vascular sensitivity. Understanding these underlying causes helps us create effective treatment plans that address not only the visible symptoms of redness but also the factors that contribute to its persistence.
While anyone can experience skin redness, certain individuals are more prone to factors such as skin type, genetic predisposition, and environmental sensitivities. People with fair skin, for instance, often have a greater tendency toward visible redness, especially when exposed to environmental triggers like sun, wind, or cold weather. Similarly, individuals with sensitive skin may find that their skin reacts easily to ingredients, products, or even changes in humidity, leading to frequent redness and irritation.
Rosacea, a chronic skin condition that affects millions worldwide, is a significant cause of this condition and is more common in adults, particularly women between the ages of 30 and 50. Genetic factors can also make certain individuals more likely to experience skin redness, especially if there is a family history of rosacea or other inflammatory skin conditions. Additionally, lifestyle and environmental factors, such as high stress levels, a diet high in spicy foods, or frequent sun exposure, can exacerbate it, particularly for those with a predisposition to it.
For those with sensitive skin or conditions like rosacea, we offer medical-grade skincare products and topical treatments that reduce inflammation, strengthen the skin barrier, and prevent future flare-ups. These products are specially formulated to soothe the skin, calm irritation, and help repair the skin’s natural protective barrier. Prescription skincare can be particularly beneficial for clients with rosacea, as these treatments are designed to manage chronic inflammation and keep redness under control.
Chemical peels can be highly effective for clients with mild to moderate redness who seek an improved, even skin tone. Peels work by exfoliating the top layers of skin, encouraging cell turnover, and reducing pigmentation irregularities that may accompany redness. We offer a range of peel strengths and types tailored to each client’s skin needs, helping to reduce it while revealing a fresher, more balanced complexion beneath.
Sylfirm X is a cutting-edge radio-frequency micro-needling treatment ideal for reducing redness, rosacea, and vascular issues. It uses dual-wave technology to precisely target blood vessels causing redness while also boosting collagen for stronger, more resilient skin. This non-invasive treatment offers minimal downtime, effectively calming the skin and reducing future flare-ups for a clearer, balanced complexion.
IPL (Intense Pulsed Light) treatment and the IllumiFacial by Lynton Lasers target redness by using advanced light technology to calm overactive blood vessels and reduce visible skin flushing. These non-invasive treatments help restore an even skin tone while promoting healthier, radiant skin with minimal downtime.