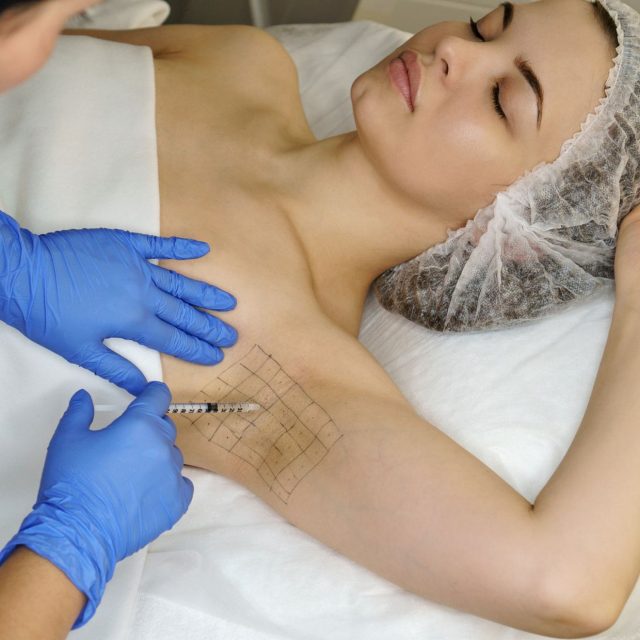
Discover the transformative benefits of anti-wrinkle injections for excessive sweating, also known as hyperhidrosis. This minimally invasive treatment offers a significant reduction in sweating, allowing you to regain confidence in every social and professional interaction.
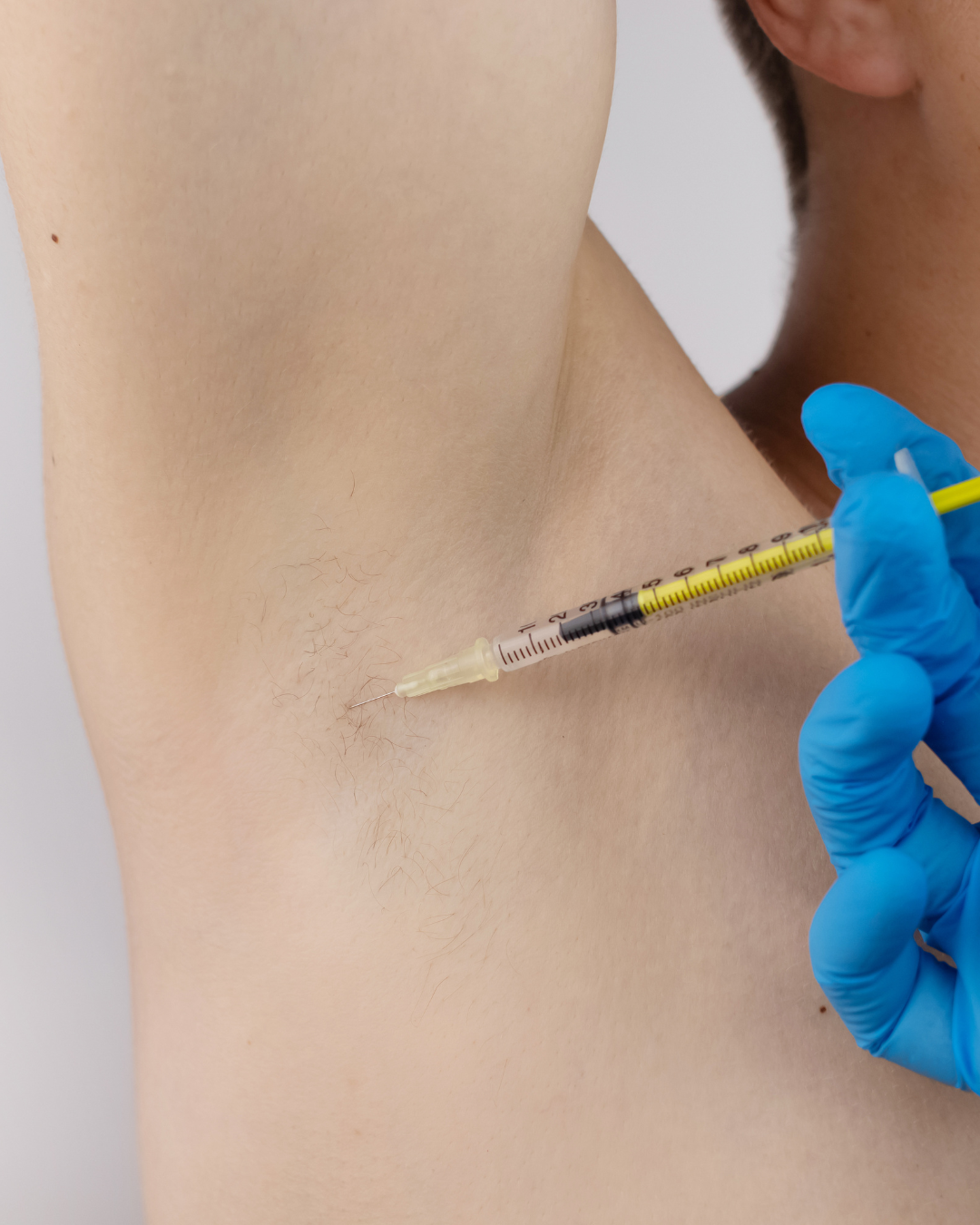
Excessive sweating can be an uncomfortable and embarrassing issue, but anti-wrinkle injections provide an effective excessive sweating treatment solution. By administering small doses of botulinum toxin directly into the sweat glands, these injections block the nerve signals responsible for sweat production, significantly reducing sweating in the treated areas.
The procedure is straightforward and typically takes around 30 minutes. Tiny injections are made just beneath the skin, usually in areas like the underarms, palms, or face, depending on your needs. Most patients start noticing results within a few days, with the effects lasting between 6 to 12 months. This means you can enjoy a sweat-free life for months without the constant worry of visible sweat patches or odour.
Anti-wrinkle injections for excessive sweating are ideal for those who find that over-the-counter solutions, such as antiperspirants, are not enough. Whether you’re dealing with hyperhidrosis in your armpits, face, or other areas, this treatment offers a safe and effective option to reduce sweating and improve your quality of life.
One of the advantages of anti-wrinkle injections for excessive sweating is its quick recovery time. Most patients can return to their normal activities immediately after the procedure, with minimal aftercare required. Unlike more invasive options, anti-wrinkle injections are a simple yet highly effective solution for managing hyperhidrosis.
To maintain the benefits of reduced sweating, treatment is generally required every 6 to 12 months, depending on your individual’s response.
Yes, anti-wrinkle injections can be effectively used on other areas prone to excessive sweating, such as the hands, feet, scalp, and face.
No, the treatment only affects the specific area where the injections are administered. Your body will still be able to regulate temperature through sweating in untreated areas.
Anti-wrinkle injections, using botulinum toxin, temporarily block the nerve signals responsible for activating sweat glands in the treated area. By stopping these signals, the injections reduce excessive sweating, giving you dry, comfortable skin for months.
Anti-wrinkle injections, using botulinum toxin, temporarily block the nerve signals responsible for activating sweat glands in the treated area. By stopping these signals, the injections reduce excessive sweating, giving you dry, comfortable skin for months.
Anti-wrinkle injections for excessive sweating cause minimal discomfort. We use fine needles, and many clients report only a mild, temporary stinging sensation. Topical numbing cream can be applied if desired.
While anti-wrinkle injections significantly reduce sweating, they may not stop it entirely. The level of dryness achieved varies by individual but most clients report a substantial reduction that improves comfort.